
Dr Curro Mirrales is speaking all about Portal Venous waveforms at #HR25 - come learn from the best!! May 22-23 in Montreal 🇨🇦. Grab your spot today!!!
ccusinstitute.wixsite.com/ccus/events/...

Dr Curro Mirrales is speaking all about Portal Venous waveforms at #HR25 - come learn from the best!! May 22-23 in Montreal 🇨🇦. Grab your spot today!!!
ccusinstitute.wixsite.com/ccus/events/...
By moving farther away to the portal vein, we can get a better reflection of organ congestion with diuresis, as was elegantly demonstrated in this recent paper
pubmed.ncbi.nlm.nih.gov/38734970/

By moving farther away to the portal vein, we can get a better reflection of organ congestion with diuresis, as was elegantly demonstrated in this recent paper
pubmed.ncbi.nlm.nih.gov/38734970/
The R-heart failure/severe TR patients are often the most challenging to assess in terms of congestion.
Many of them will ALWAYS live at a high CVP.
The R-heart failure/severe TR patients are often the most challenging to assess in terms of congestion.
Many of them will ALWAYS live at a high CVP.
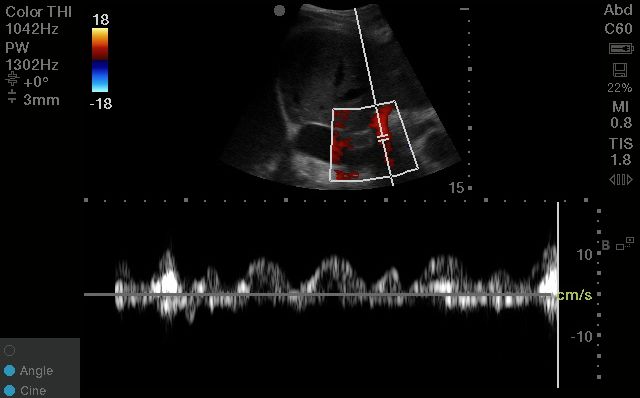
Unlike the hepatic vein, which can be misleading in the absence of EKG gating, the portal vein is easily interpreted
You can use calipers to measure pulsatility fraction; but you can also use the eyeball method to assess mild vs moderate vs severe pulsatility.
Unlike the hepatic vein, which can be misleading in the absence of EKG gating, the portal vein is easily interpreted
You can use calipers to measure pulsatility fraction; but you can also use the eyeball method to assess mild vs moderate vs severe pulsatility.
Unlike the intra-renal veins, which can be elusive even to the most experienced scanners, the portal vein is usually easily identifiable.
From R coronal plane in the mid-axillary line, with your liver/kidney in view, fan or slide your probe in the anterior-posterior plane.
Unlike the intra-renal veins, which can be elusive even to the most experienced scanners, the portal vein is usually easily identifiable.
From R coronal plane in the mid-axillary line, with your liver/kidney in view, fan or slide your probe in the anterior-posterior plane.
Come join us at #HR25! May 22-23, 2025 🇨🇦
ccusinstitute.wixsite.com/ccus/events/...

Come join us at #HR25! May 22-23, 2025 🇨🇦
ccusinstitute.wixsite.com/ccus/events/...
An intensivist, physiology enthusiast, and all-star medical educator, he'll be speaking at #HR25 all about next-level Non-Invasive Ventilation ✨
An intensivist, physiology enthusiast, and all-star medical educator, he'll be speaking at #HR25 all about next-level Non-Invasive Ventilation ✨
#MedSky #skeetorial #emimcc #InternalMedicine
#MedSky #skeetorial #emimcc #InternalMedicine
All this being said: a huge part of rounding efficiency comes from experience. As you become more comfortable managing common problems and your knowledge base expands, so too will your rounding efficiency 🧠
All this being said: a huge part of rounding efficiency comes from experience. As you become more comfortable managing common problems and your knowledge base expands, so too will your rounding efficiency 🧠
The vasculopath admitted for heart failure who has new colour change and pulselessness in their foot, in contrast, certainly does!
The vasculopath admitted for heart failure who has new colour change and pulselessness in their foot, in contrast, certainly does!
This comes largely with experience and a growing knowledge base, but knowing when something is an issue that requires further (possibly urgent) investigation, and when something can be safely deferred or observed, is a key skill 🗝️
This comes largely with experience and a growing knowledge base, but knowing when something is an issue that requires further (possibly urgent) investigation, and when something can be safely deferred or observed, is a key skill 🗝️
This is not always possible for patient care and flow reasons, but I do find it helpful ✅
For example: I will often save my discharge summaries and do these after completing my rounding on all my patients.
This is not always possible for patient care and flow reasons, but I do find it helpful ✅
For example: I will often save my discharge summaries and do these after completing my rounding on all my patients.
Having a dedicated time to discuss with Allied Health, for example; or a system whereby nurses can leave non-urgent messages for the care team (without a phone call/page), can be helpful
Having a dedicated time to discuss with Allied Health, for example; or a system whereby nurses can leave non-urgent messages for the care team (without a phone call/page), can be helpful
I know, I know - this can be next to impossible in a hospital setting, especially in certain environments. (Hats off to all my EM friends who manage near constant interruptions!)
I know, I know - this can be next to impossible in a hospital setting, especially in certain environments. (Hats off to all my EM friends who manage near constant interruptions!)
That's not to say that your plan can't change from day to day, but it makes it much easier if you've already done the initial cognitive legwork.
That's not to say that your plan can't change from day to day, but it makes it much easier if you've already done the initial cognitive legwork.

